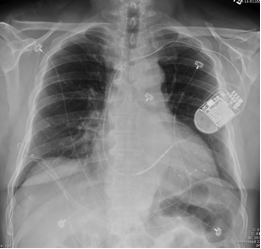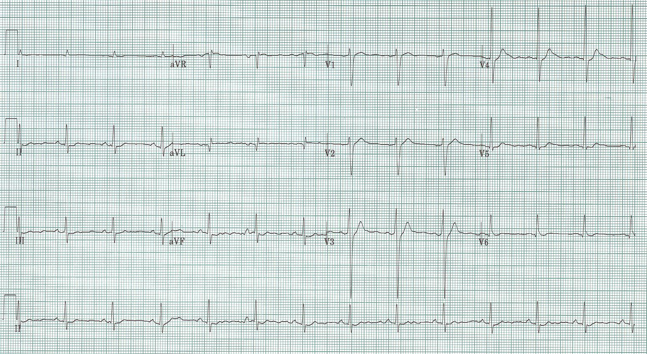
76-year-old man with squamous cell cancer of the oropharynx presents with lethargy and confusion.
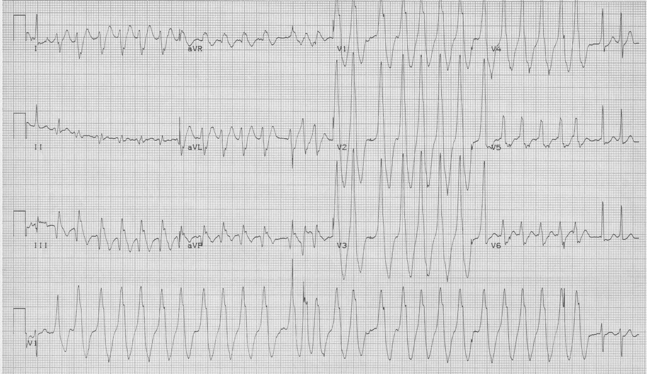
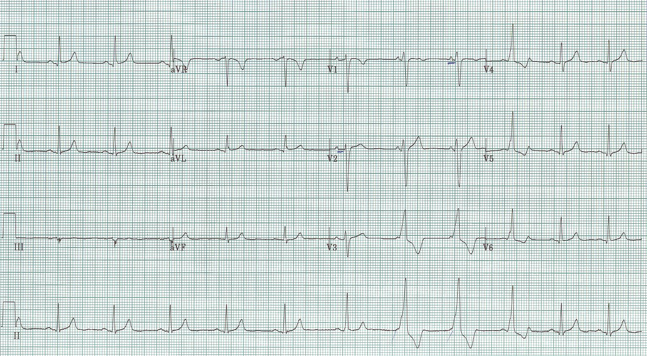
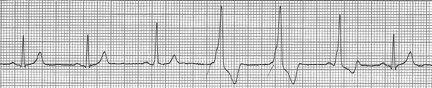
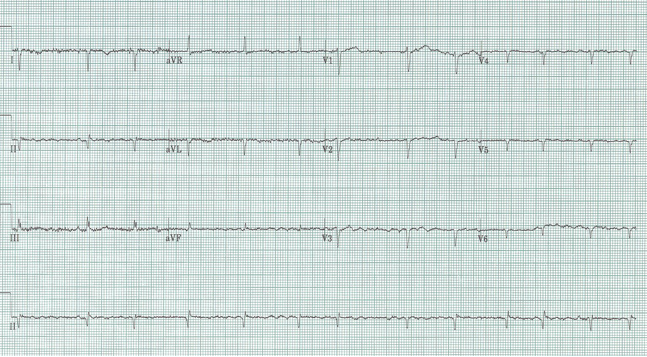
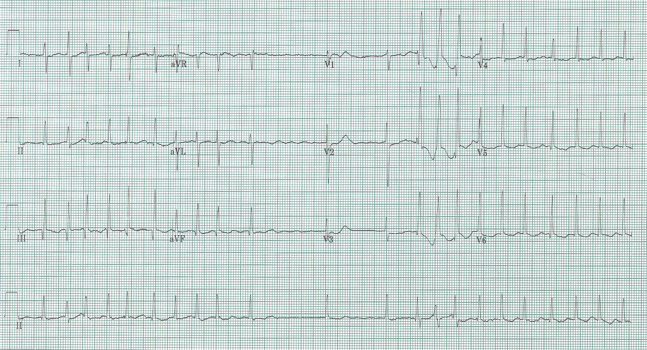
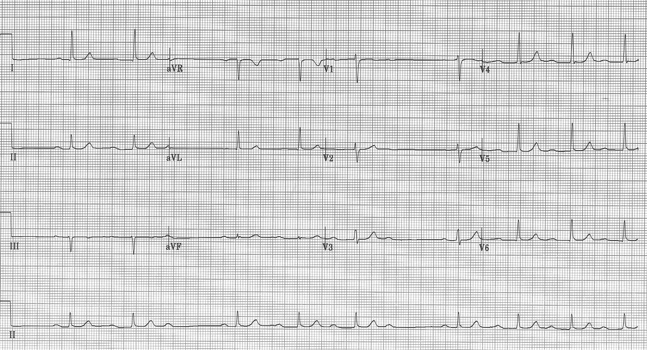
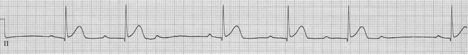
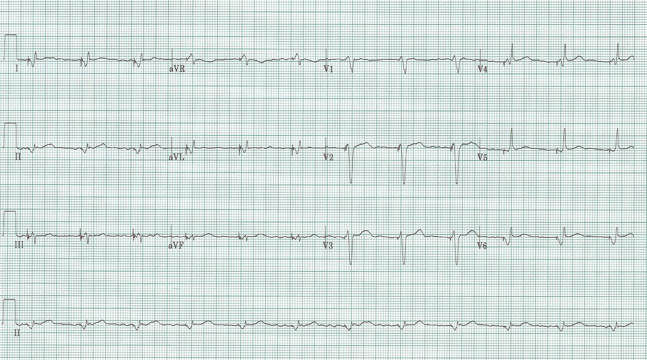
Sinus at 75/minute
Axis normal, PR and QRS also normal
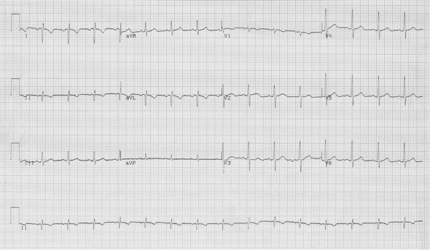
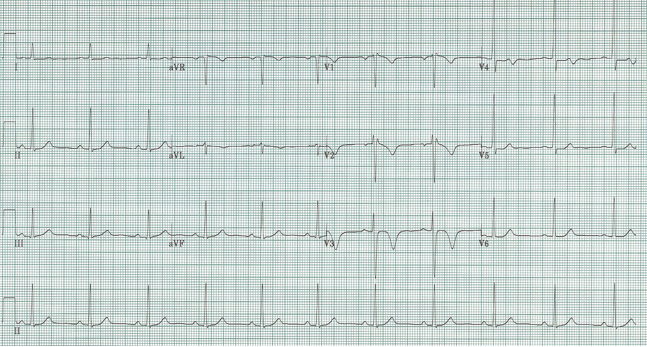
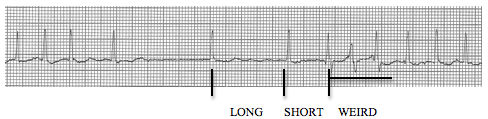
QT interval is visibly shorter than normal
No LVH
No ischemia or infarct patterns
A decrease in QT interval is seen with hypercalcemia, which fits with the patient’s presentation and known malignancy. This gentleman’s ionized calcium was 2.2.
The ST-segment is short or absent in hypercalcemia and the duration of the QTc interval is decreased. Although it is difficult to give an absolute QTc interval below which hypercalcemia is assured, this value is always <400ms and visually fairly obvious.
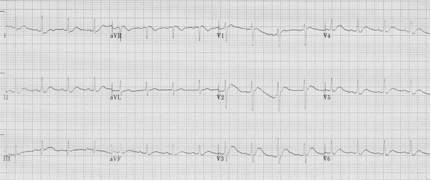
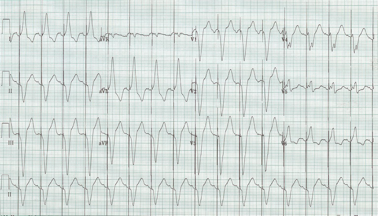
Another occasional EKG presentation of hypercalcemia is leftward movement of the apex of the T-wave as in the above example, another example of hypercalcemia associated with malignancy.
Diercks D, et al. Electrocardiographic manifestations: electrolyte abnormalities. J Emerg Med 27:153-160, 2004.